In 2022, 666,000 people died from breast cancer globally.
This year, an estimated 42,670 women and 530 men in the US will die of breast cancer.
These are just two of the statistics that speak to the urgent need to end this deadly disease.
In 2026, an estimated 321,910 women and 2,670 men in the United States will be diagnosed with invasive breast cancer, and an additional 60,730 women will be diagnosed with ductal carcinoma in situ (DCIS).* Breast cancer remains the most commonly diagnosed cancer among women.
*Annual incidence counts of lobular carcinoma in situ are no longer measured following its removal from the 2017 edition of the AJCC breast cancer staging program.
Trend over time: Breast cancer incidence increased rapidly in the 1980s and 1990s with the widespread adoption of screening, declined briefly in the early 2000s, and has risen steadily since 2012 by about 1% per year overall.

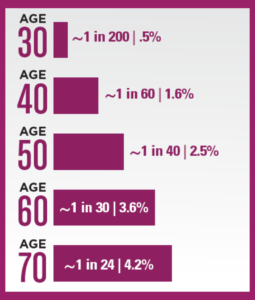
Incidence by age: Breast cancer incidence increases with age. From 2017–2021, the median age at invasive breast cancer diagnosis in the US was 63 years.
At right: chance of being diagnosed with invasive breast cancer within the next 10 years** (approximate).
**These estimates reflect cumulative risk over a 10-year period and are not annual risks.
Stage at diagnosis: Recent increases in breast cancer incidence are driven primarily by localized-stage diagnoses, while rates of advanced disease have remained relatively stable—underscoring the limits of detection alone in reducing mortality.
Lifetime risk: For women in the United States, the lifetime risk*** of being diagnosed with invasive breast cancer has increased since 1975, reflecting both changes in risk and increased detection over time.
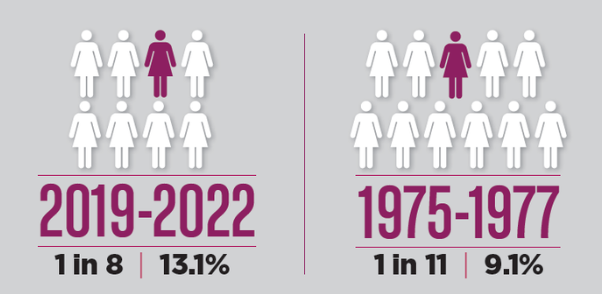
***Lifetime risk describes the probability of being diagnosed over an entire lifetime and should not be interpreted as the risk at any given age
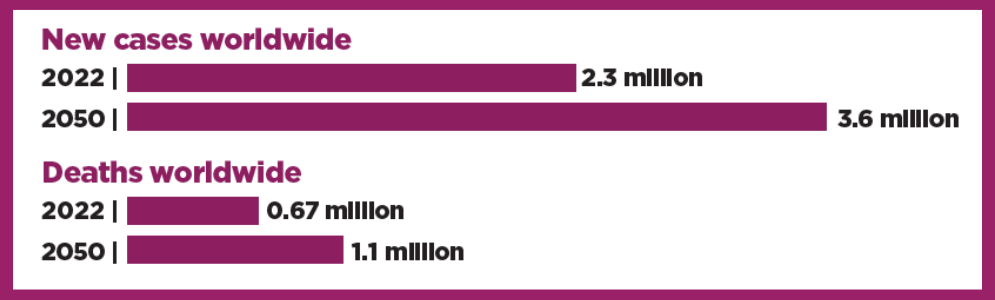
In 2022, an estimated 2.3 million new cases of breast cancer and about 666,000 deaths occurred worldwide, representing roughly 24% of all cancer cases and 15% of all cancer deaths in women.
By 2050: If current national rates remain stable, the number of new breast cancer cases and deaths worldwide is projected to increase by more than 50% and 70%, respectively, largely due to population growth and aging.
Breast cancer is the second-leading cause of cancer death among women in the US, after lung cancer. In 2026, an estimated 42,670 women and 530 men will die of the disease.
Breast cancer mortality has declined substantially since the early 1990s; however, progress has slowed in recent years—from annual declines of 2%–3% in the 1990s and 2000s to about 1% per year since 2010.
While breast cancer mortality rates have declined, the absolute number of women and men who die each year is rising and is expected to continue to rise as the population ages.
Mortality by age: From 2018-2022, the median age at death from breast cancer was 70 years, reflecting the fact that breast cancer mortality increases with age.
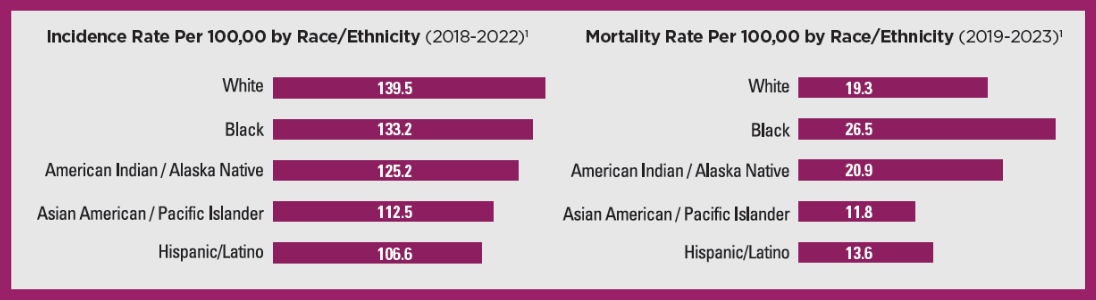
Incidence and mortality by race/ethnicity: Breast cancer burden varies across racial and ethnic groups, with lower incidence and mortality among Asian American/Pacific Islander and Hispanic/Latina women, and disproportionately high mortality relative to incidence among American Indian/Alaska Native women.
Despite lower incidence, breast cancer mortality among Black women is approximately 40% higher than among white women in the US. Although mortality rates have declined for both groups over time, this disparity has persisted, reflecting longstanding inequities in access to timely diagnosis and high-quality care.
As of January 1, 2025, an estimated 4.31 million women in the US were living with a history of invasive breast cancer.
Among female breast cancer survivors in 2025, about 7% were younger than age 50, 26% were 50–64, 56% were 65–84, and 11% were 85 and older.
Population-based estimates suggest that the number of women living with metastatic breast cancer in the US has increased from about 140,000 in 2018 to approximately 170,000 today.
Recurrence risk varies widely and depends on multiple factors.
Long-term cumulative risk estimates range from 5% to 60%, with most between 10% and 30%, and can remain elevated for more than 30 years after diagnosis.
Only 5–10% of breast cancers are caused by inherited genetic mutations.
The strongest risk factors for breast cancer: increasing age and being assigned female at birth.
Ductal carcinoma in situ (DCIS) consists of abnormal cells confined within the milk duct. The cells have not invaded surrounding breast tissue.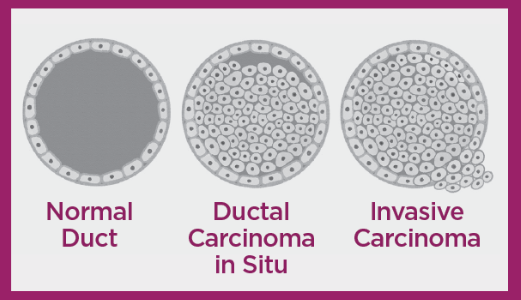
Not all DCIS will progress to invasive breast cancer. Because we cannot yet reliably predict which cases may progress, both treatment strategies and active monitoring approaches are being studied in clinical trials.
DCIS diagnosis was rare before 1980. The widespread adoption of screening mammography was associated with a substantial increase in DCIS diagnoses. From 1980–2000, women ages 20–49 experienced an approximately 400% increase in DCIS diagnoses, while women ages 50 and older experienced more than a 900% increase.
Despite this increase in early-stage detection, screening mammography has not led to a corresponding decrease in the rate of distant-stage (lethal) breast cancer at diagnosis.
Overdiagnosis of breast cancer—the detection of cancers that would not have caused harm during a person’s lifetime—remains difficult to quantify. Estimates of overdiagnosis associated with screening mammography range from approximately 11% to 22%, and may include both DCIS and some invasive cancers.
Screening mammography can also result in false-positive and false-negative findings. Over a 10-year period, more than half of women undergoing annual screening mammography will experience at least one false-positive result, leading to additional imaging or biopsy.
Common approaches to breast cancer treatment in the United States include:

A note on language: Though the literature tends to use language that reflects a gender binary, NBCC as an organization acknowledges that breast cancer affects people of all gender identities.